Strokes cause numerous changes in gene activity in affected small blood vessels in the brain, and these changes are potentially targetable with existing or future drugs to mitigate brain injury or improve stroke recovery, according to a study led by Weill Cornell Medicine scientists.
In the study, which appears April 14 in the Proceedings of the National Academy of Sciences, the researchers performed a comprehensive survey, in a preclinical model, of gene activity changes in small blood vessels in the brain following stroke. Comparing these changes to those that have been recorded in stroke patients, they catalogued hundreds of genes with significant stroke-driven changes and likely relevance in human strokes.
“Our findings provide a knowledge base that improves our understanding of strokes and points to specific molecules and pathways that can now be investigated as potential targets for future stroke treatments,” said study senior author Dr. Teresa Sanchez, assistant professor of pathology and laboratory medicine and principal investigator of the Laboratory of Molecular and Translational Vascular Research at Weill Cornell Medicine. “It is also increasingly recognized that vascular disease is associated with and contributes to cognitive dysfunction and dementia. This study has identified molecular features associated with vascular dysfunction in the human brain after stroke, a major cause of dementia.”

Dr. Teresa Sanchez. Credit: John Abbott.
Stroke is and has long been a leading cause of mortality and long-term disability worldwide. The vast majority of strokes are ischemic strokes involving a blood clot in a vessel serving the brain. The blockage or severe reduction of blood flow reduces oxygen and nutrient delivery to downstream brain cells, killing or injuring them and triggering inflammatory processes that can cause further damage.
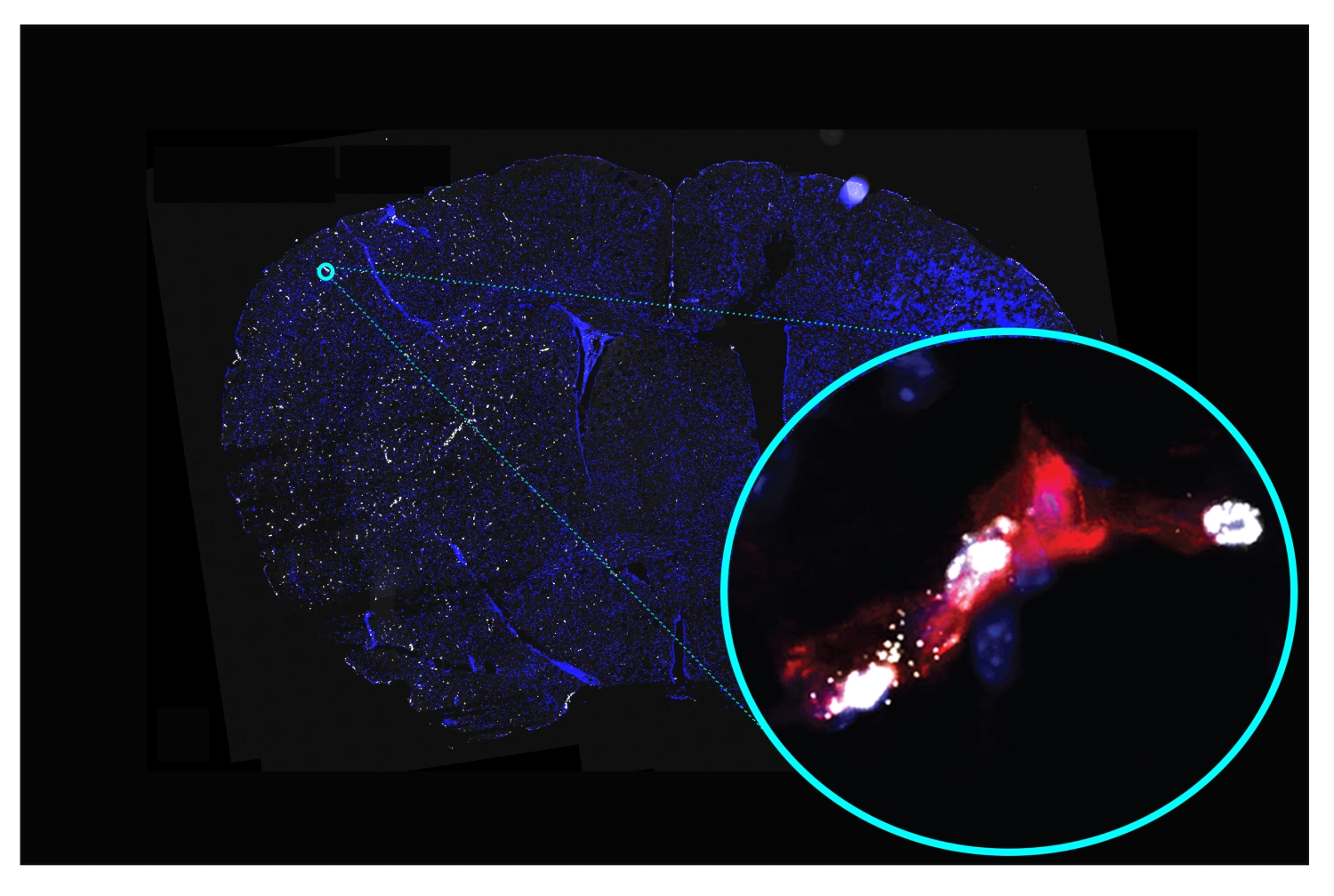
The small cerebral blood vessels—or “cerebral microvasculature”—downstream of the blockage are also affected, and the changes in them are thought to contribute further to brain damage post-stroke. Yet these microvascular changes have been technically challenging to record accurately, and thus have not been as well studied as other aspects of stroke—nor do they have any specific treatment.
In the new study, Dr. Sanchez and her team, including co-first authors Drs. Keri Callegari, Sabyasachi Dash and Hiroki Uchida, used the latest optimized methods, recently published by the Sanchez laboratory in Nature Protocols, for studying stroke-affected vessels to surmount these challenges. They comprehensively recorded post-stroke changes in gene activity in the cerebral microvasculature in mice and identified the changes that have also been seen in studies of human stroke patients.
In all, the team found 541 genes whose activity was altered similarly in both mice and human cerebral microvessels post-stroke. Dividing these genes into groups based on their functional roles and disease links, they identified several major clusters. These included clusters relating to general inflammation, brain inflammation, vascular disease, and the type of vascular dysfunction that would cause cerebral microvessels to become leaky. This leakiness implies a weakening of the “blood-brain barrier,” the cellular lining of cerebral microvessels that protects the brain by keeping most components of circulating blood out of it.
“We found that, following stroke, some molecules that would weaken the blood-brain barrier were upregulated, while others that should protect the blood-brain barrier were downregulated,” said Dr. Sanchez, who is also an assistant professor of neuroscience in the Feil Family Brain and Mind Research Institute. “This is consistent with clinical observations of blood-brain-barrier disruptions following stroke.”
The analysis also identified the disruption of normal activity in genes controlling the levels of sphingolipids. These fat-related molecules are heavily involved in regulating blood vessels, and disruptions of their normal workings have been observed in stroke, atherosclerosis and vascular dementia. The team discovered that some types of these sphingolipids are highly enriched in cerebral blood vessels compared with brain tissue. In addition, they identified alterations in these sphingolipids in the cerebral microvasculature induced by stroke as well as the changes in key molecules that control the levels of these lipids. These new findings will permit the pharmacological targeting of these pathways for stroke therapeutic discovery.
The study included assessments confirming the “druggability,” or suitability for targeting with small-molecule drugs, of many of the molecules with altered production post-stroke. Indeed, some of the identified molecules are already being targeted by candidate drugs to treat other pathological conditions, which could facilitate the repurposing of these drugs for the treatment of stroke and dementia.
Dr. Sanchez and her team are now following up with preclinical experiments using candidate drugs or genetic methods to reverse some of the specific microvascular changes identified in their study, to investigate if this could be beneficial for stroke patients.
“We’ve generated this knowledge platform and we’re using it, but we also hope that other scientists will join us in these efforts to develop the first therapies targeting the microvasculature in stroke,” she said.
Dr. Teresa Sanchez is an inventor on a patent application for a method used to identify molecular features in the human brain after stroke.