With vaccine availability growing in New York City and across the country, attention is increasingly turning to those who are eligible but hesitant about getting the shot.
Between 70 to 90% of the population needs to be vaccinated in order to reach herd immunity and bring the pandemic under control, according to public health experts. Yet 13% of Americans report they will definitely not get a vaccine, and another 24% are planning to wait and see or will only get one if required, according to a Kaiser Health News poll reported March 30.
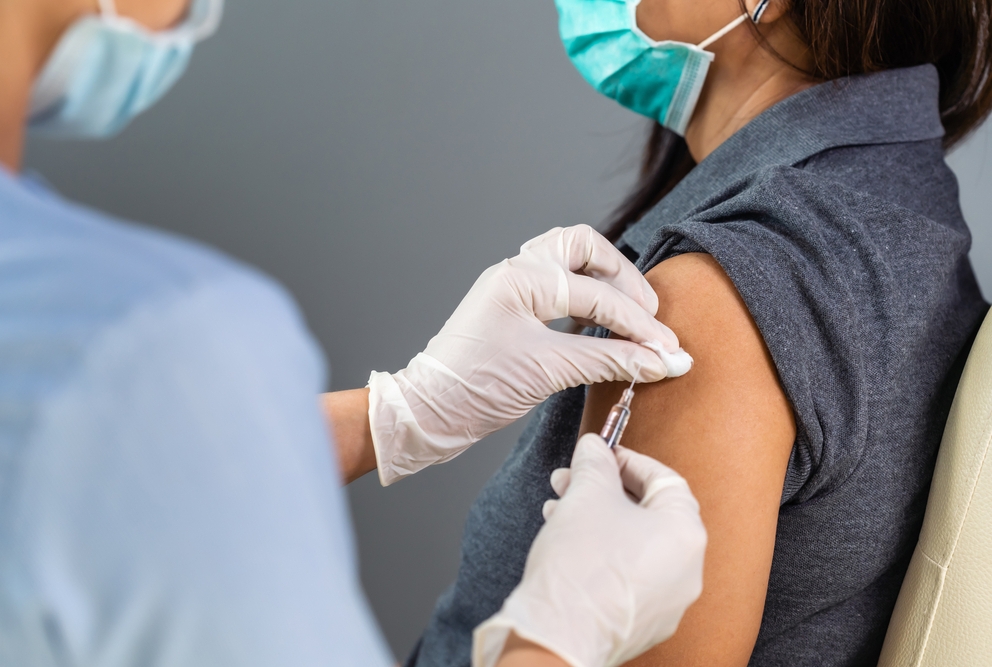
 Weill Cornell Medical College and Hunter Nursing students help administer 473 COVID-19 vaccine doses April 10 at the CTSC’s community vaccination site in Jamaica, Queens.
Weill Cornell Medical College and Hunter Nursing students help administer 473 COVID-19 vaccine doses April 10 at the CTSC’s community vaccination site in Jamaica, Queens.
Much attention has focused on hesitancy of Black and Hispanic populations, based on members of these groups’ feelings of mistrust and experience of the healthcare system. For this reason, diversity leaders at Weill Cornell Medicine launched ambitious community vaccination and education efforts early on in the vaccine rollout, with the goal of improving uptake and helping those who are reluctant overcome their concerns.
Yet recent polling suggests that slightly more Blacks plan to get vaccinated than do whites. Healthcare professionals who work with and belong to Black and brown communities say the focus needs to be as much on making the vaccine easy to access as on hesitancy.
Vaccination at Trusted Community Spaces
Although anyone over age 16 is now eligible in New York State for a vaccine, getting an appointment can require significant time online trying to find an open slot as well as time spent getting to a site and waiting in line. This puts some people at a disadvantage.
“If you don't have good WiFi, or you don’t know how to navigate the websites, you’re probably just going to give up,” said Dr. Said Ibrahim, senior associate dean for diversity and inclusion and professor of population health sciences at Weill Cornell Medicine. “The problem right now is largely access to the vaccine,” he adds, pointing particularly to supply as well as difficulty finding appointments. “It’s a little premature to call it all about hesitancy.”
NewYork-Presbyterian in January opened a vaccination site at the Armory, prioritizing appointments for eligible residents of the Washington Heights, Inwood, Harlem and South Bronx communities. Additionally, the Weill Cornell Medicine Clinical and Translational Science Center has worked with the Community Healthcare Network of federally qualified health centers to administer 2,505 vaccine doses at sites staffed by Weill Cornell Medical College students in church and non-profit spaces in the Bronx and Queens.
They plan to expand these efforts this month, joining with Hunter College nursing students to run vaccination clinics four days a week at churches in Jamaica, East New York and Harlem, with the aim to vaccinate 100,000 people by September.
Dr. Julianne Imperato-McGinley, director of the CTSC and a professor of medicine who is leading the effort with Jeff Zhu, managing director of community engagement and research at the CTSC, says it's important to make vaccination available in people's own communities, particularly at “trusted spaces,” like places of worship or a neighborhood organization. She and Zhu had previously worked with the reverend of a church and his congregation on a free health screening program called Heart to Heart. He reached out to CTSC and got vaccinated himself in front of his congregants.
“The point about community trust is essential. That’s why we’re doing this with faith-based communities, where the community knows the people hosting the event,” Dr. Imperato-McGinley said.
Reframing Hesitancy as Self-Advocacy
Historic mistreatment by the healthcare system toward communities of color has received significant attention, particularly the Tuskegee experiment in which researchers withheld penicillin from Black participants to treat syphilis, as well as other violations of research ethics in experiments involving racial minorities, low-income people, incarcerated people, or the disabled. But it’s not just history, say experts. COVID-19 has had a disproportionate impact on communities of color, and some from these groups report mistreatment today and remain underserved by the healthcare system.
For this reason, questions about why vaccines—which usually take years to develop— could be produced so quickly, or whether they could cause side effects in the future, should be seen as self-advocacy rather than hesitancy, public health experts have said. To help healthcare professionals respond to people’s questions and concerns, in March Weill Cornell Medicine trained “vaccine ambassadors” as relatable, credible sources of information.
“It’s not about convincing people. It’s about providing information that is sorely missing. It’s about empowerment and access,” said Dr. Susana R. Morales, associate professor of clinical medicine at Weill Cornell Medicine and director of the institution’s Diversity Center of Excellence within the Cornell Center for Health Equity, who spearheaded the ambassador training. “Physicians of color are amongst the trusted messengers in communities of color because of histories of mistreatments,” she adds. She notes that many people who have not yet gotten their shots may not be strongly opposed to doing so, but are “not willing to run over someone,” to get vaccinated.

Weill Cornell Medical College and Hunter Nursing students help administer 176 COVID-19 vaccine doses Feb. 27 at the CTSC’s community vaccination site in Jamaica, Queens.
At the training, panelists framed conversations with patients, family and others who are hesitant as filling a "knowledge gap,” and advised approaching questions in a receptive and empathetic manner.
"What I tell patients is, ‘I promise you I’ve done the research about COVID vaccinations to decide whether I can recommend vaccines to you and whether I was going to accept the vaccine myself,’” said Dr. Morales, who shares with patients that she has been vaccinated.
In response to concerns about the speed of vaccine development, Dr. Morales said she describes how clinical trials were able to enroll thousands of diverse volunteers and produce results quickly because of how widespread the virus has been. Additionally, given the scale of the pandemic, regulatory agencies prioritized review of the vaccines, and governments and manufacturers invested heavily in their development.
Ambassadors address questions about vaccine side effects by noting study participants continue to be monitored for serious adverse reactions, which investigators must report, and drug makers and other study sponsors must disclose. They also point out long-term side effects of COVID-19 infection such as neurological damage, which the vaccine protects against. To patients from populations that weren’t included in vaccine studies who have questions, like pregnant women or those on chemotherapy, ambassadors can share findings from the latest research. For example, none of the currently approved vaccines have shown negative effects on fertility rates or pregnancy abnormalities in animal studies and early data on vaccinated pregnant women is very encouraging, according to panelist Dr. Kevin Holcomb, associate dean for admissions and professor of clinical obstetrics and gynecology. While cancer patients on chemotherapy may not experience as robust an immune response as others, Dr. Holcomb said during the March ambassador training, a vaccine is better than COVID-19 infection for people who are immunocompromised.
Dr. Holcomb said he has also tried to talk to people about the historical comparisons, when appropriate. He has discovered some are under the false impression that in the Tuskegee study, researchers infected Black participants with syphilis, when in fact they denied them penicillin to treat the disease.
“What happened in Tuskegee is what we might be doing by not availing ourselves of this vaccine,” Dr. Holcomb said.
Driving Dialogue on Vaccines
The COVID-19 STEM Community Education and Empowerment Internship, another effort Dr. Morales recently launched, will bring together Weill Cornell Medicine and other area medical schools this spring and summer to train undergraduates interested in medical and health careers on the vaccine and addressing hesitancy. More than 770 students from 28 states, Puerto Rico, Washington, D.C., and three other countries have enrolled in the internship. For the capstone project, students will create social media campaigns or presentations about the vaccine targeted to lay audiences and will commit to speaking to at least 10 people about getting vaccinated. “Even if we only have 300 per cohort, that’s 3,000 people we’ll reach,” Dr. Morales said.
Weill Cornell Medicine’s recent Diversity Town Halls, hosted by the Office of Diversity and Inclusion, have also centered around vaccination. In January the event featured former leaders of the National Medical Association, the oldest and largest Black physician organization, speaking about the history of vaccine hesitancy among racial and ethnic minorities, and a second in March included faith leaders who are working to educate their congregants about the vaccine.
While there has been a strong focus on hesitancy among groups of color, currently Republicans and white evangelicals are the most likely to say they won’t get a shot, with close to 30% of each group holding this position, according to the Kaiser poll. Among nearly all groups, hesitancy has dropped significantly since the rollout began late last year. Blacks now are just as likely as whites to say they’ll get the vaccine, at 73% compared to 70%, according to a survey reported March 12 by NPR, PBS NewsHour and Marist.
Perhaps surprisingly, one of the most hesitant groups are healthcare workers. Megan Downes, a registered nurse and clinical quality and patient safety manager at Weill Cornell Medicine who spoke at the March Diversity Town Hall, says they often have a “wait-and-see” approach.
After considering concerns, such as potential side effects, Downes ultimately decided to get vaccinated. “I was weighing the risk of getting COVID and what that might mean for me and my family health-wise, versus taking a chance on the vaccine,” she said. “So I came down on the side of the vaccine.” Now, as a registered nurse and a Black woman, she’s trying to have conversations with people she knows who have what she says are legitimate questions about the vaccine.
“We need advocates who look like me to be part of the system,” Downes said. “I try to be honest about what isn't known about the long-term effects but also focus on what we do know. What I can do is try to set an example and answer questions, and try to encourage others to do the same.”