For Pierre Georges Bonnefil, the morning of February 6, 2013, started off like any other. He made coffee for his wife, Marysia, and watched the news before getting ready for his job as an immigration attorney. But then Marysia noticed something was wrong: the left side of Bonnefil’s face had begun to droop and he suddenly couldn’t move his left arm. “I started to speak, but she said it made no sense whatsoever,” says Bonnefil. “That’s when she put two and two together and called 911.”

Pierre Georges Bonnefil in his Manhattan apartment, where he suffered a stroke several years ago. Photo credit: John Abbott
Bonnefil was having a stroke, a condition that affects nearly 800,000 people in the United States every year. According to the Centers for Disease Control and Prevention, one American dies from a stroke — which happens when blood flow to the brain is interrupted — every four minutes, making it the fifth-leading cause of death and a major cause of serious, long-term disability. Rushed from his midtown Manhattan apartment to NewYork-Presbyterian/Weill Cornell Medical Center — ranked among the country’s top institutions for advanced stroke care — Bonnefil was diagnosed with a middle cerebral artery (MCA) stroke, meaning that one of the largest blood vessels in the brain was blocked. “It was pretty much as bad as it gets,” says Dr. Babak Navi, assistant professor of neurology at Weill Cornell Medicine and medical director of the Weill Cornell Medicine Stroke Center, who treated Bonnefil at the hospital.
But Dr. Navi says Bonnefil was luckier than most: because his wife recognized the signs and called for help right away, he was given a clot-busting drug just 74 minutes after his symptoms began. Getting swift medical attention also meant he was able to receive endovascular therapy, a procedure that involves inserting a catheter into the brain to remove the clot. Bonnefil went home five days later; although he attended outpatient physical therapy for three months to strengthen the left side of his body, he was back to most normal activities within weeks. “He came back very quickly — that doesn’t always happen,” says Dr. Navi. “Stroke is incredibly time sensitive, arguably more than any other disease. Each minute that a typical stroke goes on, patients on average lose about two million brain cells. So every minute counts.”
Racing the Clock
Bonnefil is a prime example of how early intervention is critical when it comes to stroke. Neurologists often use the phrase “time is brain” when talking about the disease, since it’s well established that the sooner patients receive treatment, the better off they’re likely to be. Even short delays can make a big difference: a 2014 study by the American Heart Association found that stroke survivors lose an average month of healthy life for every 15 minutes of postponed treatment. Weill Cornell Medicine, with heavy support from NewYork-Presbyterian, began leading a study of a mobile stroke treatment unit, the first of its kind on the East Coast. The unit, launched also in collaboration with Columbia University Medical Center and the FDNY — does more than reach stroke victims quickly: it also provides a pipeline of subjects for time-sensitive clinical trials being conducted at Weill Cornell Medicine, as well as other research initiatives that may lead to new therapies.

Dr. Babak Navi. Photo credit: Studio Brooke
The unit is a customized emergency vehicle that brings a highly specialized team of experts, diagnostic equipment and stroke-specific drugs right to a patient’s doorstep. “The key to treating stroke patients is getting to them as early as you can, as fast as you can, and this unit makes that possible,” says the program’s executive director, Dr. Matthew Fink, neurologist- in-chief and chief of the Division of Stroke and Critical Care Neurology at NewYork-Presbyterian/Weill Cornell Medical Center and the Louis and Gertrude Feil Professor and chairman of the Department of Neurology at Weill Cornell Medicine. “But this is just the beginning. I view this unit as something transformational that may dramatically change the way we deliver care.”
The unit is deployed in the neighborhoods surrounding NewYork-Presbyterian/Weill Cornell at East 68th Street and NewYork-Presbyterian/Columbia at West 168th Street, where a combined total of nearly 2,000 stroke patients come for aid every year. Staffed by a neurologist, two paramedics and a radiology technician, the unit is dispatched weekdays between 7 a.m. and 3 p.m. when an emergency call comes in to New York City’s 911 system and operators suspect a stroke. (Eventually, those hours of operation will be adjusted based on the times when most stroke calls come in.) Unlike a traditional ambulance, it includes a portable computed tomography (CT) scanner that can image a patient’s brain on the spot, so the medical team is able to determine whether a stroke is ischemic (caused by a blood clot) or hemorrhagic (which occurs when a weakened blood vessel ruptures). For ischemic strokes — which account for 87 percent of all stroke cases — vital medications can be administered immediately, such as the one Bonnefil received called tissue plasminogen activator, or tPA, which is considered the “gold standard” for recovery. If patients receive tPA within four and a half hours of the onset of symptoms, they have a much greater chance of surviving and avoiding long-term brain damage; after that, the drug offers no benefit.
Thanks to the unit, a neurologist sees stroke patients immediately, rather than waiting until they get to the emergency room. While en route, the doctor can signal ahead to hospital colleagues, who can be poised for additional tests or alternate remedies as soon as a patient arrives, further streamlining the process. (Eventually, the on-board neurologist will shift to being on call at the hospital; he or she will use telemedicine to evaluate those picked up by the unit without delay, using a remote audio-visual system to ask questions and examine the patient and CT scans in real time; this way, neurologists can still determine treatment for stroke patients more quickly, and attend to other tasks while waiting for a call to come in.) “The conventional ambulance system was never designed to treat out in the field; patients aren’t seen by a doctor and don’t undergo testing until they get to the hospital,” says Dr. Fink, who first proposed the mobile program two years ago. “The mobile unit essentially becomes an extension of the emergency department.”
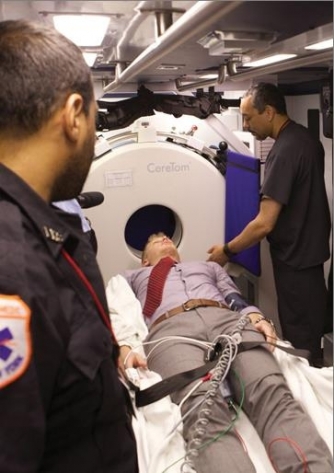
The specially equipped ambulance is designed to diagnose and treat stroke. Photo credit: NewYork-Presbyterian
New Yorkers at Risk
Advanced stroke care is particularly important in places like New York City, which has a growing population that is becoming increasingly elderly and ethnically diverse. African Americans, Asian Americans and Hispanics have a higher chance of dying or being disabled from stroke than whites, in part because of genetics and other contributors that increase the likelihood of risk factors such as hypertension and diabetes. And though the disease affects people of all ages, the risk of having a stroke is far greater as one gets older. According to the city’s Department for the Aging, as a result of demographic shifts, the number of older whites living in New York dropped by nearly 10 percent between 2000 and 2013, while minority members of that age group shot up by 55 percent in that same period. In addition, the total number of seniors is projected to increase to 1.86 million by 2040, which means that one in every five New Yorkers will be over age 60 by then. “After the age of 50, the risk of stroke doubles with every decade,” says Dr. Fink. “So that’s a major problem, because people can reduce or eliminate some risk factors, but we can’t change our age.”
Indeed, on only its second day in operation, the stroke unit responded to a call from a doctor’s office on the Upper East Side, where a woman in her 90s had come in for a routine checkup. While there, she began to feel dizzy and weak on one side. The unit’s medical squad sped to the site and was able to give the woman tPA within the “golden hour,” so named because the treatment is even more powerful if administered within 60 minutes of the onset of symptoms. That’s rare; only about 1 percent of stroke patients nationwide receive tPA in that ideal window. As a result, she made a complete recovery. “It was a moment that made me proud to be a doctor,” says Dr. Mackenzie Lerario, the mobile stroke unit program’s medical director and an assistant professor of clinical neurology at Weill Cornell Medicine, who treated her. “We can come in and treat patients quicker and more effectively than we ever could before. It’s an elegant solution to a complex problem.”
The concept of the mobile stroke unit originated in Germany, where physicians who studied this method reported in 2012 that it reduced time to treatment by about 25 minutes compared to regular emergency transport. Subsequent studies have also shown significant time reductions at the Cleveland Clinic and the University of Texas Health Science Center in Houston, where the first U.S. mobile stroke units began operating in 2014. Researchers are still investigating whether these shorter response times directly correlate to improved outcomes, but earlier this year a group of doctors in Berlin published an article in Lancet Neurology that seems to support that theory. Their study found that patients treated by mobile units had a lower death rate and less severe disabilities three months after a stroke than those who received conventional care.
Weill Cornell Medicine, Columbia and NewYork-Presbyterian are collecting data to assess their own unit’s efficacy, tracking patient information such as mortality rates, degree of disability, length of hospital stay and type of complications for up to a year after initial treatment at either facility. Health expenditures are being examined, too, to determine the value of such units for academic medical centers and healthcare systems, including the feasibility of expanding to include additional units and incorporating mobile care into insurance reimbursement models. “I think that’s highly possible because if you’re preventing disability by giving tPA to patients quicker, the patients who are less disabled are going to use fewer healthcare resources in the future,” says Dr. Lerario. “They’ll have fewer rehabilitation needs. They’re going to be admitted to the hospital less frequently with complications of stroke.”
To Dr. Fink, these mobile units open up even bigger possibilities. Not only do they have the potential to radically improve stroke outcomes, he says, they could represent a shift in how providers deliver overall emergency care. “Right now we’re doing this for stroke, but I can imagine that this might extend to other kinds of emergencies like heart attacks or trauma — where we treat patients out in the field and not wait until they come to the hospital,” he says. “This might be the first of many new developments in taking the hospital out to the patient.”
UNIT FUELS NIH TRIALS
Investigators are using the mobile unit as a way to enlist patients for clinical trials in stroke prevention, acute stroke treatment and stroke recovery that are now under way as part of the NIH’s StrokeNet network of 25 regional stroke centers across the country. Weill Cornell Medicine doctors are studying such topics as whether endovascular therapy, which is usually only done within six hours of stroke symptoms, could benefit patients treated between six and 16 hours of onset; and whether a drug typically used to remove excess iron from the body might work to reabsorb blood in the brain after an intracranial hemorrhage.
Dr. Navi is Weill Cornell Medicine’s site principal investigator for StrokeNet’s POINT (Platelet-Oriented Inhibition in New TIA and Minor Ischemic Stroke) trial, which aims to determine the safety and efficacy of a combination of low-dose aspirin and another blood-thinning drug in reducing the risk of stroke, heart attack and other complications in patients who have already had a transient ischemic attack (otherwise known as a mini-stroke) or a minor ischemic stroke. “Many of the stroke patients who come in through the mobile unit may be eligible for these trials, so it allows us to identify, recruit and enroll them quicker,” says Dr. Navi. “By studying these interventions, the more likely we are to identify a new treatment that we can provide to the stroke community at large.”
EXPLORING STROKE’S CAUSES
As clinicians improve care for stroke patients, scientists at Weill Cornell Medicine’s Feil Family Brain and Mind Research Institute (BMRI) are examining a wide range of topics involving the condition. The institute’s director, Dr. Costantino Iadecola, says one major goal in the clinical arena is to figure out what causes strokes that are classified as cryptogenic, or of unknown origin; this is imperative, he says, since one-third of ischemic strokes fall into this category and people who have already had a stroke are more likely to have another one. “If we can identify the cause, we are in a better position to prevent future strokes,” says Dr. Iadecola, a professor of neuroscience and the Anne Parrish Titzell Professor of Neurology. “Therefore, finding a cause can have a profound impact on how we take care of these patients.”
To do that, Dr. Navi and Dr. Hooman Kamel, an assistant professor of neurology, hope to identify new risk factors, such as subtle dysfunctions of the heart, as well as the association between stroke and cancer. In addition, the institute’s basic science researchers have found that cells of the immune system are crucial; Dr. Iadecola and his colleagues now know that certain immune cells can dramatically help reverse post-stroke brain damage, while others appear to exacerbate it. Another recent discovery, headed by Dr. Josef Anrather, a professor of neuroscience, indicates that bacteria normally present in our gut can also help repair stroke-induced brain damage. Dr. Iadecola notes that these findings could lead to promising new treatments, ones that may also need to be given to stroke patients quickly. If that’s the case, he says the mobile stroke unit could play a central role in testing early-stage interventions. “Should our science suggest that we have a new drug or a new therapeutic approach, we now have a way to deliver these novel treatments early,” says Dr. Iadecola. “It opens up new horizons for stroke therapy.”
— Heather Salerno
This story first appeared in Weill Cornell Medicine, Vol. 16 No. 1.

