Laparoscopic surgery is poised to revolutionize liver donation
When Gina Vintalore learned that her cousin might die of stage-three cirrhosis while waiting for a liver transplant, the solution seemed obvious to her. "I asked him if he had considered a living donor," she says, recalling their conversation at a family barbecue. "He said, 'Who would I ask?' I said, 'Well, I would do it.' "
Living donations, in which the donor provides between 20 and 60 percent of his or her liver, are possible because the organ has a unique ability to regenerate. But historically, potential donors have faced risks to their own health, along with the certainty of a large scar and a recovery period lasting some two months. It's not surprising, then, that of the 6,000 liver transplants performed each year, only 5 percent use living donors.
Vintalore, however, faced a much less daunting procedure — thanks to Dr. Benjamin Samstein, who has pioneered a first-in-the-nation laparoscopic program with the potential to shorten recovery time, reduce complications, and make living liver donation far more common. For donors, the minimally invasive procedure involves instruments inserted through a few small incisions, rather than open surgery. It means less pain, less fatigue, and faster healing. "I was running 10 days later," says the 48-year-old Vintalore, who underwent a 12-hour surgery in August to remove the right lobe of her liver, which was transplanted into her cousin. A few days after that, Vintalore — a physical education teacher in Paterson, N.J. — was back at work in time for the start of the school year. "It was a very quick recovery," she says. "I'm back to 100 percent."
Dr. Samstein, the new chief of liver transplantation and hepato-biliary surgery at Weill Cornell Medicine, has so far performed the laparoscopic procedure on about 30 organ donors. He hopes that the new approach will increase the number of liver transplants and save lives. "One of the challenges is that most donors don't spontaneously come to the center; somebody has to approach them," Dr. Samstein observes. "If you have to undergo surgery and a recovery that will take two to three months, I'm less likely to ask you to donate an organ. If that recovery is shortened to two weeks, I'm more likely to ask."
As the risk and recovery time for the donor decreases, Dr. Samstein explains, patients feel more comfortable accepting an organ from a stranger or asking an acquaintance or a coworker for help if close relatives cannot donate — and those people will be more willing to oblige. That's what happened with kidney donation, where more than a third of transplants come from living donors, and where laparoscopic surgery is now routine. "Liver transplant has less experience than kidney transplant," Dr. Samstein says, noting that the first successful kidney transplant took place in 1954, with a living donor. While the first liver was transplanted in 1963, the organ came from a deceased donor. Moreover, the operation only became routine in the '80s, and the first liver transplant from a living donor didn't happen until 1989. "I think of liver transplant as being about 30 years more junior to kidney transplantation," says Dr. Samstein, an undergraduate alumnus of the Ithaca campus. "That's why, I think, there is so little knowledge, and why some doctors might not even present living donation as an option."
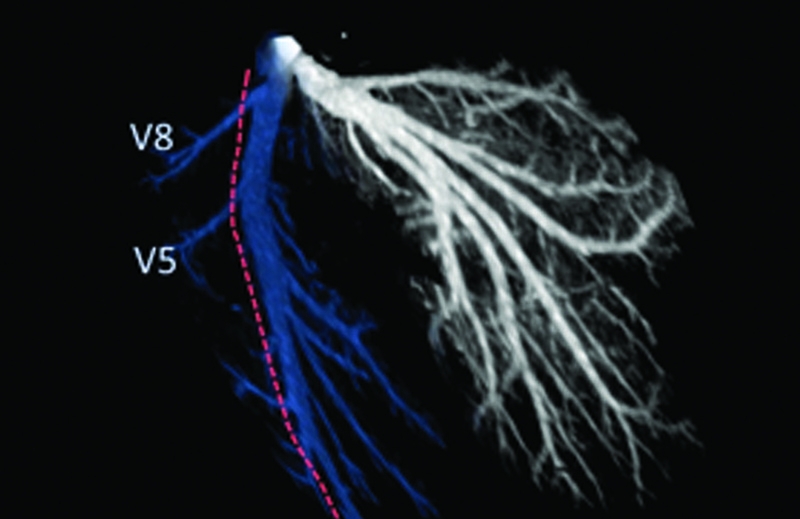
Kinder cut: An image of the left and right hepatic veins, and (in red) the line of transection for liver transplant. Image credit: Dr. Benjamin Samstein
NewYork-Presbyterian is currently the only hospital system in the United States to offer laparoscopic surgery for liver donors, but Dr. Samstein hopes that distinction will not last. He and his team recently published a paper in Annals of Surgery documenting their success, and they've been working to understand how the procedure might be made less technically challenging, so it could be performed at more centers. That would encourage more donations and allow more people in need to get livers — good news for the 18,000 patients on the national waiting list for livers from deceased donors. Every year, some 1,500 people die waiting for a liver. "The need for organs far outstrips our access," Dr. Samstein says. "Our overarching goal is to increase the number of transplants."
He also points out that the current system for allocating organs prioritizes the sickest patients, even though transplant recipients clearly fare better when they receive new organs sooner, with survival rates up to 40 percent higher. "In order to have the best outcome, it's not clear that giving organs to the sickest people is the only appropriate way to do it," Dr. Samstein says. "Living donation enables somebody to get a transplant when it's determined that they need one, and not only because they are the sickest person on the list."
For Vintalore, who recently had her cousin over to dinner and watched with delight as he held his 2-year-old son on his lap, the donation was undoubtedly worth it. She chuckles as she recounts the efforts Dr. Samstein and the Living Donor Advocate Team at NewYork-Presbyterian/Weill Cornell Medical Center took to ensure she was psychologically prepared for the experience — and her efforts to assure them that she was just glad she could help. "I did not have a moment of hesitation," Vintalore says. "I'm laid up for what, a couple of weeks? And he gets to live. It's a no-brainer."
— Amy Crawford
This story first appeared in Weill Cornell Medicine, Vol. 15, No.1.